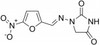
Nitrofurantoin is broad-spectrum nitrofuran antibiotic that is used as a substrate for bacterial glycoprotein nitrofuran reductase. It is bacteriostatic against Gram-positive and Gram-negative bacteria. The compound has been found to have anti-cancer properties against bladder cancer cells grown in vitro. The product can be used to study antibiotic resistance.
Nitrofurantoin is soluble in DMF but practically insoluble in aqueous solution.
We also offer:
- Nitrofurantoin Sodium (N061)
| Mechanism of Action | Nitrofurantoin has a unique mode of action in that it does not require growth or active metabolism to exert its effect. Upon entering a susceptible cell, Nitrofurantoin is activated by bacterial enzymes (nitrofuran reductase) and targets ribosomes and nucleic acids which inhibit bacterial growth and leads to death of the bacterial cells. Resistance to Nitrofurantoin may be chromosomal or plasmid-mediated. |
| Spectrum | Nitrofurantoin is a broad-spectrum antibiotic frequently used to treat bacterial infections of the urinary tract. Nitrofurantoin has been found to be effective against certain β-lactam resistant strains of VRE or vancomycin resistant Enterococcus; a glycopeptide antibiotic resistant "superbug." Nitrofurantion is also used against Enterococci, Staphylococci, Streptococci, Corneybacteria, and E. coli. Most strains of Proteus spp. and Pseudomonas aeurginosa are resistant to Nitrofurantoin. |
| Impurity Profile | Limit of Nitrofurfural Diacetate: ≤ 1.0% Limit of Nitrofurazone: ≤ 0.01% |
| Microbiology Applications | Nitrofurantoin is commonly used in clinical in vitro microbiological antimicrobial susceptibility tests (panels, discs, and MIC strips) against Gram-positive and Gram-negative microbial isolates. Medical microbiologists use AST results to recommend antibiotic treatment options. Representative MIC values include:
Nitrofurantoin can be used against Lysteria monocytogenes-persisters in vitro, and was effective against both growing and dormant cells (Knudsen et al, 2013). In general, organisms are said to be susceptibile if the MIC is ≤ 32 µg/ml. The activity of this compound is pH- dependent, and the mean MIC rises sharply with pH >6. Microfluidic droplet systems are popular analytical methods used in antimicrobial susceptibility testing (AST) to help study antimicrobial resistance (AMR). Droplet methods have many advantages over conventional AST methods. Authors used several antibiotics from TOKU-E including Nitrofurantoin to review the physicochemical properties to predict retention of antibiotics in droplets (Ruszczak et al, 2023). |
| Eukaryotic Cell Culture Applications | Nitrofuranton is toxic to human WI-38 fibroblasts in culture and antioxidants can mitigate effect. On a molecular basis, glutathione peroxidase was the most efficient at protection (Michiels and Remacle, 1988). Nitrofurantoin can alter the morphology, viability, and phagocytic activity of bovine mammary polymorphonuclear leukocytes in vitro, when added at 1 mg/ml (Nickerson et al, 1995). |
| Cancer Applications | Nitrofurantoin was evaluated for cytotoxic activity against bladder cancer cells using three transitional cell carcinoma lines (HTB9 (grade 2); T24 (gr 3) and TccSup (gr. 4) at 0-2000 µg/ml using the MTT assay. Significant, dose-dependent cytotoxicity was seen at 7.8 µg/ml in all 3 cell lines (Kamat and Lamm, 2004). |
| Molecular Formula | C8H6N4O5 |
| Solubility | Soluble in DMF. Practically insoluble in aqueous solution. |
| References |
Fitzpatrick PM and Charles C. McOsker CM (1994) Nitrofurantoin: Mechanism of action and implications for resistance development in common uropathogens. J. Antimicrob. Chemother. 33(Suppl A):23-30 PMID 7928834 Kamat AM ad Lamm DL (2004) Antitumor activity of common antibiotics against superficial bladder cancer. Urol. 63(3):457-460 PMID 15028437 Knudsen GM, Ng Y and Gram L (2013) Survival of bactericidal antibiotic treatment by a persister subpopulation of Listeria monocytogenes. App. Environ. Microbiol. 79(23):7390-7397 PMID 24056460 Nickerson SC, Paape MJ, Dulin AM (1985) Effect of antibiotics and vehicles on bovine mammary polymorphonuclear leukocyte morphologic features, viability, and phagocytic activity in vitro. Am J Vet Res. 46(11):2259-2265 PMID 4073636 Ruszczak A, Jankowski P, Vasantham S, Scheler O and Garstiecki P (2023) Physicochemical properties predict retention of antibiotics in water-in-oil droplets. Anal. Chem. 95(2): 1574−1581 PMID 36598882 |
| MIC | Bacillus cereus (ML 98)| ≥25|| Bacillus subtilis| 1 - 12.5|| Bordetella bronchiseptica| >400|| Burkholderia cepacia| >400|| Edwardsiella hoshinae | 2 - 8|| Edwardsiella ictaluri | 1 - 4|| Edwardsiella tarda| 4 - 8|| Enterococcus faecalis| 8 - 12.5|| Enterococcus spp.| ≤32 - >64|| Escherichia coli| 4 - >64|| Helicobacter pylori| 1 - 2|| Klebsiella pneumonia| ≥25|| Klebsiella spp.| ≤32 - >64|| Lactobacillus acidophilus| 1 - ≥256|| Lactobacillus brevis| 16 - ≥256|| Lactobacillus casei| 64 - ≥256|| Lactobacillus curvatus| 128 - ≥256|| Lactobacillus delbrueckii| 8 - ≥256|| Lactobacillus fermentum| 32 - ≥256|| Lactobacillus gasseri| 1|| Lactobacillus johnsonii| >100|| Lactobacillus paracasei| >100|| Lactobacillus plantarum| 32 - ≥256|| Lactobacillus rhamnosus| 64 - ≥256|| Lactobacillus sakei| 128 - ≥256|| Lactobacillus salivarius| 10|| Lactobacillus sp.| 4 - 256|| Listeria spp.| 8 - >64|| Pediococcus acidilactici (HA-6111-2)| ≥16|| Proteus vulgaris| ≥100|| Pseudomonas aeruginosa| >64 - >400|| Shigella| 1 - 32|| Staphylococcus aureus| 2 - 25|| Stenotrophomonas maltophilia| ≥400|| Vibrio harveyi| 6.25|| |